Next month it will be officially five years since my son was diagnosed with eosinophilic esophagitis (also known as EOE, previously known as EE). We’ve tried lots of things and settled into our rare disease life. Because of the publicity of this blog, I often receive lots of questions about how we’ve handled it, and so I thought it’d be helpful to share what we’ve done and learned along the way, in one easy-to-find article.

*Please note that this was just our experience, and that I in no way think this is the one and only way to handle the treatment of this disease. This is merely to help you see how another family has managed the disease and give you talking points to discuss with your own doctor as you decide your own care with practiced medical professionals. This post may also contain affiliate links.*
What is eosinophilic esophagitis?
The American Partnership for Eosinophilic Disorders (a super helpful resource!) defines it as: “…a chronic, allergic inflammatory disease of the esophagus (the tube connecting the mouth to the stomach). It occurs when a type of white blood cell, the eosinophil, accumulates in the esophagus and persists despite acid-blocking medicine. The elevated number of eosinophils cause injury and inflammation to the esophagus. This damage may make eating difficult or uncomfortable, potentially resulting in poor growth, chronic pain, and/or difficulty swallowing.”
I often describe it in plain terms like this: My son has regular food allergies, and because of a rare disease his esophagus also has allergies. If he eats the foods that triggers his esophageal allergies, then it damages his esophagus and can cause him pain, his esophagus to swell, and even cause food to get stuck.
What were his symptoms?
This is the most frequently asked question, and I’ll go into detail to be helpful. Around 2 months, my son started getting big, red rashes on his cheeks after I’d nurse him (see pic below). He also had mucous in his stools and they were extremely runny and he’d have blow outs after every diaper (note–diaper issues alone don’t always mean there is anything wrong) and machine-gun-like gas.
We were told that he most likely had an immature immune system and for me to go on an elimination diet to see if there was anything that I was eating that was bothering him, since he was exclusively breastfeed. I don’t know why, but my pediatrician chose (because these are not the top-8-allergens, but rather an odd assortment): dairy, nuts, eggs, whole grains, citrus, corn, strawberries, tomato and chocolate. She had me take all of those out for two weeks to clear my system, then I would bring in one food at a time (starting with chocolate and working my way backwards). I’d eat that food for three days–if my son didn’t react to them, then they were considered OK to keep in my diet.
He ended up reacting to eggs, soy and wheat–so I avoided those for the year that I nursed him.
As we started giving him more and more solid foods we noticed that he did not care for them, and that he vomited frequently. The rashes on his cheeks often came back, and his weight percentiles started dropping. He was almost off the entire growth curve by the time we were able to see his allergist.
How was he diagnosed with EOE and how old was he?
The only official way to be diagnosed with EOE is to have an EGD (Esophagogastroduodenoscopy–also known as a scope) taken with biopsies, and then a pathologist looks at the biopsies to see if there are eosinophils present in the tissue.
Up to this point, at eleven months, my son had had an anaphylaxic reaction to the first time he had dairy, and with his history of also needing eggs, soy and wheat taken out of my diet while nursing him, my allergist decided to do blood work. His blood eosinophil count was so high he said he might either have EOE or leukemia and that either way we needed to get him scoped soon. –Note–blood work does not always match what is going on in the individual tissue of the esophagus, so this was just a predictor, but tissue samples must always be taken to know how the particular area is doing.
Allergists cannot preform an EGD, so we went and found a pediatric GI doctor to do the procedure. After it was done, and a pathologist confirmed and he was given the diagnosis of EOE at 14 months old.
How does your child do after an EGD (scope)?
He does great. I believe he has a high pain tolerance, and that they aren’t the worst procedures. They are quick–15 minutes or so is all they’re under–and the instrument that they use to take the samples, I’ve been told, is like the size of the tip of your pen. I’m sure the pain level also varies depending on how damaged your esophagus is, and how many they have to take, and how long it’s been since your last scope. There was one scope where he said he had been bleeding after he took a sample because it was fragile, and he ended up vomiting because of the blood on his empty stomach when he came out of anesthesia. He is always drinking before he leaves the hospital, and then we try to give him soft foods for about a day–but other than Tylenol (and sometimes he doesn’t even care for any) he is fine.
How did you figure out his EOE triggers?
This is a tricky question–as it can feel like finding a needle in a hay stack. Plus, recommendations have changed since we first started. But, below is how we went about it.
Our allergist from Primary Children’s in Salt Lake City was running off of the Cincinnati Hospital’s recommendations (one of the top EOE clinics, other than Denver) to do patch testing. So, literally at least twice a week (unless his back needed to heal) we were driving 45 minutes each way to have my son first undergo prick testing–to make sure that the foods were not going to cause an anaphylaxic reaction. If he passed that, then we would patch test him. He’s had over 100+ foods tested on him (I stopped counting after 100), as we were told he had to have every single thing he’d ever eat tested to. It was long and arduous. My poor son spent the majority of his second year in a doctor’s office. He got to the point that the prick testing for anaphylaxis didn’t even phase him. He wouldn’t even flinch when he’d get the poke. He is the definition of a trooper.
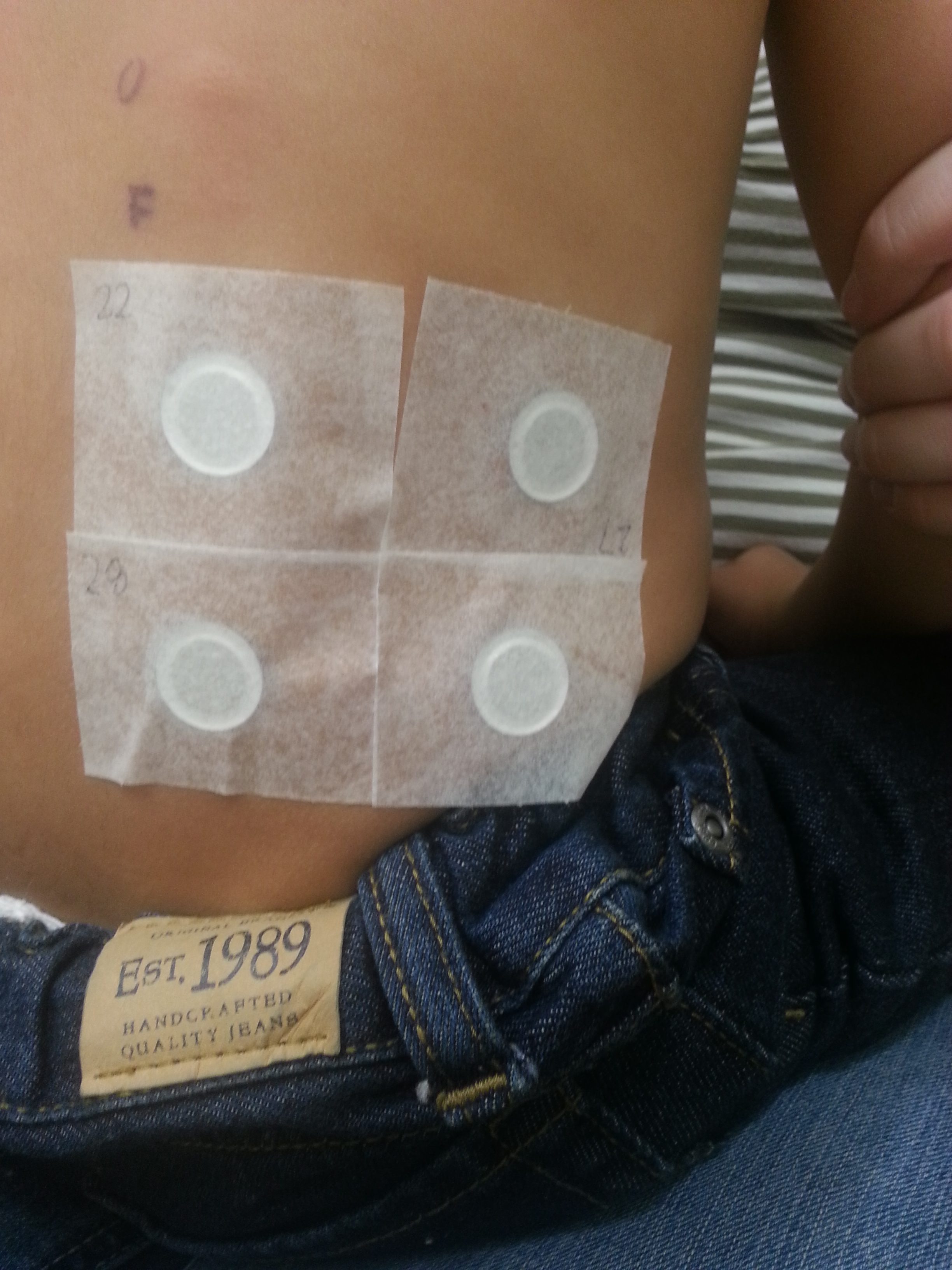
For those unfamiliar with patch testing, (also known as atopy patch testing) it is where they take the actual food and make a paste with it (I was never told the proportions of food to saline), place it on a little disc and then tape that disc to your back. They would put a control one with just saline, and then foods on the other discs. I was bringing in grocery bags of food for things they didn’t have in the office, and my allergist let me prioritize what foods and in what order we tested, according to what I’d cook with most.
The premise of patch testing was to see how skin tissue would react to a prolonged exposure to the food protein–to try and mimic how the esophagus handles foods. We would have to leave these patches, with a bunch of tape stuck to his back for two days. We even did it over summer. The poor kid could not swim or bath during this time, and he was so good to not itch. He’d honestly cry the most when I’d take it off since it’d pull his fine back hairs. I’d dread it and we’d both tear up. Man, those were hard months.
Two days after them being placed, I’d take them off at home, and take pictures (some doctors make their patients come in, but our doctor didn’t make us drive that far since he trusted how I’d handle it). Then, you let it air out for a day (no bathing). You finally go in on the third day and have them “read”. If there was raised skin, redness or irritation, that was considered a fail.
If my son passed both prick and patch testing, he was allowed to try the foods orally. Keep in mind–he had tried lots of fruits and vegetables in purees as a baby–but now we felt that they were “safer” for him to consume and might not possibly trigger his EOE and cause damage to his esophagus. Even though he had eaten a decent number of foods we re-tested EVERYTHING so that we weren’t assuming anything. Since, whatever he had previously been eating was causing damage.
Since we could get quite a few on his back at one time, we would fill it up, as to not waste an appointment. Then, if he passed any (there were fails every time–those were some disappointing 45 minute drives home. I’d often call and cry to my mom or best friends). We’d allow him to eat that one single food once a day, for several weeks, keeping track of any reactions to his skin, bowls, eating habits or throwing up. (Doing that for each food he passed.)
Thankfully, we only had one time when we got to the oral stage that seemed to affect him negatively, which was green beans of all things. It caused him horrible constipation, so we just considered that a fail and didn’t bother continuing to feed it to him or scope him.
I should mention that most medical literature nowadays does not recommend prick or patch testing as they feel it does not correlate. I do feel it was helpful for us (it is known to have a higher success rate in children than adults)–for example, he had a horrible reaction to mustard, one we would have never guessed and after several years of avoiding it we tried giving it to him again and he was clearing his throat and coughing for days. That said–I think we were one of the lucky few as most people did not feel it was helpful. It would have saved us a lot of time and hassle not having done it–but we were doing was told was cutting edge at the time (although I always thought–who in the world came up with taping food to someone’s back??).
Do you scope to more than one food at a time?
Yes. And, we understood that this was a gamble. Because, if he were to fail, we would have no idea what food caused the fail. Because of lots of prayer, mother’s intuition and because we were so careful with our approach and calculated by the time we got to foods he was eating regularly and ready to scope we felt he was doing fine, and would pass and just wanted confirmation. We felt we had weeded out the bad ones by that point, if that makes sense. There is nothing wrong with doing it the slower way, but where he was down to so few foods we took the risk. It’s a totally personal decision.
Also–we try and never scope when it’s high pollen season, since there is the idea that swallowing pollen can also cause a reaction. So, we tried to wait until winter when we can rule that factor out as well.
What do you think helped you the most?
Support, support and knowledge. We had a good team of doctors, an allergist who specialized in EOE with a GI who could pass notes to each other since they were both a part of the same Primary Children’s. We had a great dietitian (more on that later) and really great friends and family who were willing to sympathize and listen to me cry on the long drives home. They were also willing to alter what we ate when we’d do get-togethers to show further support. I joined two local support groups–one for EOE and a general food allergy one (Utah Food Allergy Network) that had yearly conferences. I made friends with moms who had been dealing with EOE longer so I could bounce ideas off of them. I also joined several support groups online on Facebook so I could ask questions to a broader audience. And, without my faith in God and His purpose and plan for me and my family I wouldn’t have made it through so many disheartening times.
Would you recommend a dietitian for EOE?
Yes. But, not all dietitians are created equal. We found one who was used to pediatric patients with limited diets–that way she wasn’t questioning why he was down to ten foods but was bent on figuring out how he could get his daily needs met. She would have me keep a dairy of all the foods he’d eat in three days. This would include every ingredient and how much. Then, she’d calculate from that how much iron, protein, vitamins…etc. he was getting. Then, she’d calculate what he was deficient on and how we could meet that (multi-vitamins, iron supplements, fortified rice milk, more quantity…etc.). It was so comforting to know that even if he was limited that he was still growing (she’d weigh and measure him every time with just his underwear on) and getting enough nutrition. It really gave me peace of mind.
Has your son ever had a feeding tube due to EOE?
No, but close. And, this can be common, especially if you’re put on elemental formula. When he was down to such a little number of foods, we were suggested to go on the elemental formula so many EOE patients are on. But, I was hell bent (maybe for the wrong reasons–because now I realize that they can be a huge help) to spend my time in the kitchen than have him get a feeding tube.
Thanks to our dietitian we realized he was OK, and since we were testing so often and constantly adding foods–first ten, then twenty, then all of the sudden fifty safe foods!–we knew he’d be OK. Plus, he was old enough and had been nursed long enough we knew he wouldn’t drink the elemental formula, so he would most likely have to be on the feeding tube and would not accept it orally since it tastes so horrible.
I’m grateful we didn’t have to put him through it, but I really had a perspective change when an older friend who had horrible eating problems said–if you didn’t have to deal with the pain and hassle of eating if it’s such a tortuous process, a feeding tube can be such a Godsend. I know there’s a lot of stigma, and I was once there myself, but now I realize there really is a time and a place for them.
How did you make sure he was getting enough calories?
Dietitian, blending his food, adding oils–is the simple answer. We tried to do anything extra fatty. Full fat coconut milk. Chicken thighs and dark meat versus chicken breasts. We were the opposite of dieting. As I mention elsewhere, we’d blend up his food, which allowed us to give him black beans, chicken, asparagus and brown rice in one sitting, whereas as a toddler he definitely wouldn’t have eaten those things on his own. Plus, we’d add at least a Tablespoon of olive oil to the purees to beef up the calories.

Waiting to be taken back to surgery.
Are you glad you tested him for EOE so young?
Absolutely. He didn’t know he was eating different and he hadn’t gotten a taste for foods yet, so he didn’t realize if he was getting a food taken away. Every year he becomes more socially aware of what others are eating, and I think it was the best blessing in disguise to have him diagnosed so early. And, since he was our first I had nothing but time to devout to him and getting this figured out before my other children came along.
How often would you scope?
I’ve heard everything and anything for frequency of scoping. We would do about every 6 months, or when we felt we had enough foods to trial. Now that our diet hasn’t changed much, we were going for once a year. However, my son has had 6 scopes, and is old enough now that he is begging for not another scope for awhile. So, we’re going to try going two years in between, mostly because we want him to get used to advocating for his health–and if we teach him to do so, and then ignore his requests we feel that is conflicting for him. We would require it, if his health seemed bad, but he has seemed stable, so we feel OK putting it off–that is a very personal, and expensive choice to make.
Should I join a support group for eosinophilic esophagitis?
Absolutely. Just be sure to only use it as needed. Some people get on there to vent and complain, which is needed sometimes, but you need to make sure you’re filling your life with positivity during such a hard time.
I’m a newbie–what is the difference between avoiding a food for anaphylaxis and EOE?
My son has both, and we avoid the foods at different levels. We avoid his anaphylaxis foods at all costs–no cross contact (meaning, you can’t use the same knife, cutting board, etc…with an unsafe food and then use it to prepare my son’s food because trace amounts can cause a reaction.)
With EOE triggers, I am still careful, but if he were to accidentally ingest one–it doesn’t seem to bother him if it’s trace amounts one time. And again, this can vary greatly from patient to patient–and especially between adults and children (for some reason there seem to be different symptoms between the two age groups). I’ve heard of some people who can have an impaction (food getting stuck in their esophagus) from eating something just once, and then some people it takes several times and it’s more of a slow build up to affect their esophagus. I know some people (mostly adults) that even cheat here and there on special occasions.
For example, my son shouldn’t have pepper for EOE. But, if we go out and I notice it’s still on his food since most people salt and pepper food without thinking, we’ll allow it. And, because we so rarely eat out–he’s never had a problem.
Whereas, if there was some cheese on my son’s food and he was to ingest it, he’d need an epi-pen and have to be rushed to the ER. So, that is a silver lining that it’s not life threatening and often not immediate. It’s also a double-edged sword since sometimes you’ll think a food is safe, but after eating it for awhile, you’ll start to notice it’s finally built up enough to realize it’s bothering you and now a trigger for EOE. It’s a lot of paying attention and vigilance to see how your own body reacts.
So, what CAN your son eat? What are his specific EOE triggers?
I keep a list of his safe and unsafe foods on my site.
How do you help ease symptoms if there is an Eosinophilic Esophagitis flair?
My son has only had one time where he felt something was stuck and seemed to be super bothered. Sometimes he will have some throat clearing, but it never seems to persist. I’ve heard of parents saying Ibuprofin, Maalox, Pepcid/Zantac helps with the tummy pain, and swallowed flovent (my son also has asthma so we always have this on hand) can help ease symptoms, but honestly–that is definitely a question for your doctor as I am not qualified to prescribe.
Has your son ever been on steroids for the treatment of Eosinophilic Esophagitis?
Right now, there are many people, especially adults–(my uncle was one of them–oddly enough, through marriage and not a blood relative) that manage the disease by taking some sort of swallowed steroid, with the thought that as you swallow it, it will coat your esophagus and help heal the damage being caused by the food or environmental allergies. They choose to do this versus change their diet either at all, or not as drastically.
I didn’t personally feel good putting my son on daily steroids at such a young age, since we were heard there is a potential to affect your adrenal system, so we chose to manage it through the diet route. Since this is a fairly new disease, and we don’t know what the long term affects are of swallowing steroids, I didn’t feel comfortable. That said–if he was not getting better after altering the diet, who knows what we would have done. It’s such a complicated and personalized disease that you can’t knock how others are choosing to cope with it.
After my son’s first scope, where we found out he had it, and the doctor showed us (he takes pictures every time he prints for us) how bad the damage was, that we put him on a two week stint of a swallowed budesonide slurry (where you pour liquid budesonide and mix it with sugar to help it be swallowed–though with the sugar you then have to watch and be careful for candida) to help his esophagus heal at a faster rate since at that point he was barely on the growth chart and hardly eating. He was only 14 months and couldn’t explain how he was feeling, but by his refusal to eat, we figured he wasn’t feeling that well. He was certainly a happy baby–in fact, you wouldn’t believe he had a disease, but we figured he was just so used to feeling crappy that he didn’t know any different and we had to look for cues like food refusal.
Did having EOE affect other areas of growth?
For us, yes. He was delayed in crawling, walking and speech. We ended up doing therapy for all of the above as well as feeding therapy. It’s hard to say since he was so young if he would have been delayed anyways, or if he felt so crappy that it hampered his development. All I can say is that he completely caught up and is now in mainstream school with no difficulties. He loves sports and tests well in school–so don’t worry if you have a small one behind, with work you can catch up!
What if I suspect my child has Eosinophilic Esophagitis, but my doctor is not taking me seriously?
I always suggest starting with your pediatrician if there are concerns. If you feel the concerns are not being validated, and that there are true issues, then you can go ahead and see if you can be seen by a specialist on your own. That is what we did. We were told, “Well, some kids are just small” and, “Well, he sleeps fine and is so happy, he’s probably fine” and so on, and so on. But, that’s what mother’s intuition is for. I’m glad I pressed and I’m glad I advocated–which was hard for me because I shy away from confrontation. One thing that helped me be taken seriously was to journal his symptoms, have a food diary (see above) and to come in with a prepared list of questions. When they saw I wasn’t just giving general complaints and how seriously I was taking it, it helped them to realize that there might be more going on than a first time, worried mom.
I feel so overwhelmed, how will I alter our diet & lifestyle as well as manage this?
I was fortunate that this was my first so I could pour a lot of time into it, I won’t deny that. And, it definitely consumed me and I let it bother me a lot.
One of the best pieces of advice I was given was to grieve the loss of foods. I remember hearing he couldn’t have spinach anymore and this was when spinach was the big rage–spinach smoothies were hot and it was touted as a “superfood” and I remember just going home after he failed it on the patch test and just bawling. Bawling over spinach! Who would have thought there was such a thing. But every food feels SO precious when they’re being taken away one by one.
Don’t distract and learn to sit in your emotions so they can pass through you instead of letting them bottle up. Easier said than done, and something I am still working on.
I think one of the best things we can do for the emotional toll is to find your tribe. If your friends and family don’t get it–find those who do. With online communities of Facebook and everything else–find people whether near or far who can validate you. Search by hashtag, ask around at doctors offices and find people who get it. I found an in-person support group in Salt Lake City which has been invaluable. Attend APFED conferences in person and by all means DON’T STOP SELF CARE. You have to take care of you in order to give. And, one thing I wish I’d learned a long time ago was to surrender. I didn’t realize the power in this until lately, and recommend to every stressed out momma this podcast (and many more of hers) to help me lift my perspective and not be a victim to my circumstance.
Do you recommend changing a lot at once in their diet?
No! For that first scope, our pediatric GI told us not to change anything, otherwise how would we see if something was going on?
I hear this a lot and think, “Oh, no! How will you know what caused them to get better or worse if you change more than one thing??”
I think that is one of the most frustrating things is that you truly have to be slow but steady. If you fail a scope and then change their diet and put them on PPIs–how will you know if it was the diet or the PPIs that made the difference? (PPI stands for proton pump inhibitor and is thought to help somewhat and also help in case there is acid reflux going on as well.)
Even though we would scope to more than one food, we’d only ever introduce a new food one at a time and keep close tabs on how it affected him before ever moving onto another one. We’d only scope when we were pretty sure he’d pass and still wanted to make sure that what we were seeing on the outside matched what was going on in the inside, since that’s the only way to be sure.
For example, after we had gone down to like ten foods right at the first we expected an improved scope and it was worse! I was devastated. I thought for sure we’d have to cut all foods. Then, we started paying attention to his food journal and noticed that he often got rashes after I’d give him spinach smoothies. And, I noticed that I had started putting spinach in all of his food blends (at that time he was still mostly puree), so that made sense why his scope was worse because instead of having an offending food every once in awhile, he was having it EVERY DAY. Once we took spinach out and scoped again he was clear. Which is again, why food journals are SOO important because it’s hard to keep track of everything and remember far back.
How did you decide what to originally cut out?
I honestly don’t remember–and it was mostly doctor driven. I remember him asking me what he had eaten a lot of to that point and used that as a base. Then, we tried to pick an assortment–so it was something like rice for a whole grain, chicken for protein, black beans for protein, carrots for a veggie and apples for a fruit and a few other things. Thankfully he scoped clean to those, so that was our base and from there we started the long testing to healthy foods I thought would improve his diet and that he’d eat and what would be seasonal/easy for me to get all year round. I was also sure to test to spices to make sure that if we had to have chicken ALL THE TIME that we could at least flavor it differently.
How did you get him to eat the same, limited diet all the time?
Age was a big factor. He was used to bland foods since he was just a little over one, and he was used to purees. That’s why I pushed and dedicated so much time at the first to figuring it out before he had the social recognition to realize how different he ate.
We got a good, quality Blendtec blender so that we could throw in all of the safe foods he could eat and still get a smooth, non-chunky smoothie or puree. It’s been life saving. It also allowed for us to sneak in broccoli and asparagus (some of the first green veggies he passed) to make sure he was getting adequate nutrition without having to deal with textures and the looks of things.
Again–having spices has been a big help, so we could do dry rubes, or just sprinkle something on. If you want to have more options, just be ready to fast track trialing foods and scoping as often as you can (while still following procedure.)
What did you include in your food journal?
I just made an easy, homemade one in Excel. It would have the date, meal times and what he ate. Then, I’d mark whether he had it more than once that day (so we knew how much of it he was getting). I’d mark whether he had any type of skin reaction, bowl reaction or throat reaction (difficulty swallowing, throat clearing) or any vomiting. And, an extra box for just any miscellaneous reaction we noticed.
Can I do this? Can we do this?
Absolutely. This will feel hard at first, but I promise you will adjust. I promise your child can still thrive. I promise this won’t be so overwhelming. Give yourself some grace and an adjusting period. One thing I tell myself constantly and my son is that “we can do hard things”. One of the many wonderful things about having a Primary Children’s hospital to go to, is seeing the VAST array of diseases and hardships other children face. When I want to cry about my son having his 7th scope, I look over and see children missing limbs, or not being able to walk. And, it helps put things in perspective. He may have to eat different, but he can run, jump, speak and do sooo much. I would say we have a very happy life and you can too. Hang in there! Good luck my friends.
What do you feed your child who has eosinophilic esophagitis?
This is exactly why I started this blog. I try to not make it messy by having too many informational posts, and keep it to recipes. I talk about the personal side mostly on my social media. So, be sure to follow me there and watch my stories as I share things as they come up. Be sure to check out my recipe index that has over 200+ recipes for free that are almost all top-8-free. (A few use soy since we can do that one.)
If you’re more into having hard copies, I have a published cookbook that you can purchase on Amazon. You can find out more about it here, including a recipe index of exactly what’s in it. Click here, or click on the photo of it below.
I also have an e-book that has the first two weeks of dinner ideas being top 8. The first two weeks can be the hardest, so I wanted those covered for you. It includes a shopping list. Click here to be taken to it, or click the photo of it below.
I Still Have Questions.
Currently my husband and I do live question and answer sessions on my Instagram and Facebook pages. You are always welcome to ask us there. You can also try emailing me (and depending on my volume and work load I will try to respond.) You are also welcome to comment below and see if others in the community can answer. And, you can also try some of the links I’ve included in the post as well.
Here is the live Q&A we did specifically on EOE. It’s almost an hour full of helpful information other readers asked.
DON’T FORGET TO PIN THIS, SO YOU DON’T LOSE IT!

Hi! I’m Megan, a mom to four kids, two with multiple food allergies & one with EOE. I’m a published cookbook author who constantly tweaks recipes to make them allergy-friendly—it’s an addiction. I’m also a member of the Allergy Advisory Council for Certified Free From Foods, where I help advocate for safer labeling and standards. I share every recipe & tip with the hope that they help you as you manage your food allergies & dietary restrictions. You can still be awesome, even with food allergies!

















Liz
I know this post is a bit older, but I’m about 4 months into the journey with my almost 3 year old. I’m trying to figure out how a go to list of processed foods (e.g. chips, chocolate bars, etc.) that I can depend on for convenience. I cook a ton, but as you all know, the drive through is never an option. Do you have any posts on this? Specifically low sugar, high calorie, filling, minimally processed foods. We love unreal coconut bars, but I think they might be causing cross-contamination issues. 🙁
Megan Lavin
Hi Liz, we don’t worry about cross contamination since EOE is not anaphylactic. I don’t worry as much about sugar as it sounds maybe you do because my main priority is filling my son up and with so many allergens something has to give. I have a list on breakfast ideas: https://allergyawesomeness.com/allergy-friendly-breakfasts/
And snacks ideas: https://allergyawesomeness.com/gluten-free-dairy-free-snacks/
Since I don’t know your son’s allergens, I hope that this helps or gets the juices flowing.
Shelley
Hi Megan,
My 14yr old son was diagonsed with EoE last week and I’ve put him on the top 8 elimination diet and the thing I’m finding most tricky is what to pack for the “lunch” part in his school lunchbox. I would be so greatful if you could please list a few things you pack in your childs lunchbox just to give me a head start.
Thank you so much.
Megan Lavin
Hi Shelley. Lunch is really difficult, especially packed lunches. I think this post will help you: https://allergyawesomeness.com/food-allergy-school-lunch-ideas/
Anne
I am the parent of a 17 year old. I am a “Been there done this for a long time” parent. Mine has resolved EOS ( From strict elimination) and anaphylactic food allergies to 13 foods. So we take no chances. Basically lunch is a 2 cup wide mouth thermos that has left overs from previous home meals. Anything goes. Sandwiches are not an option for us. He used it be concerned (when younger) of people making fun of him never having the same type things they were eating. Then he learned some were actually wishing they had what he had. I also cook multicultural: modified European, Hispanic, Asian, but interestingly not to much traditional American because allergies include wheat eggs etc. NO school food is an option in our case. When he has after school meetings and sports (he runs track) he has a second yeti thermos rated for holding heat for longer term. preheat the thermos by filling with boiling water. Use a canning jar funnel to fill it. Just a note: teach your kids to read ingredients labels as soon as they can read, AND get them involved in the kitchen reading recipes and learning how to modify them for their needs.
Sonya
Hi there. I came across your blog after my 23 month old was diagnosed with EoE. I have a couple questions that Im struggling with finding answers for. First, how long after starting treatment did you notice symptoms were improving or disappeared? We are going on 10 days post nexium and oral budesonide and my son maybe has improved in eating more snack food but still doesnt eat much at meal times. He drinks just fine of course. Secondly, did you ever doubt the biopsy results? I just wonder if my sons count could have been caused by something other than EoE.
Megan Lavin
Hi Sonya, I can totally understand why you’d want those questions–but every situation is so unique, that I really can’t give a blanket statement. According to my son’s doctor, my son’s esophagus was in such bad shape that we needed to do the swallowed budesonide for two weeks to help it heal. I can’t pinpoint a time when he started doing better, as it seemed gradual. It could also be because we were constantly tweaking his diet and so that was all going on simultaneously. I have heard that counts can be off, if they miss a high power field, but you can always ask for the samples to be sent to another lab to be re-looked at by someone else. Best of luck! Wishing you success on this frustrating journey.
Megan
HI Megan, I’m also Megan and was recently diagnosed with EOE and am on the Six Food Elimination diet of the top 8. Thanks for sharing your story. its hard to find others that are going though the same thing so it’s nice to connect.
Megan Lavin
Hi Megan! Nice to e-meet another EOE person. Wishing you the best on your journey.
Jamie Taliaferro
I’m just finding this blog/website and I am very grateful! My son is 10 now and started reacting to foods (that I noticed) at 7 months when he threw up peas. That was the start of our EOE journey and it’s been extremely difficult at times. He had GERD from birth so more than likely was born with EOE, unfortunately. He did not get officially diagnosed though until he was about 7 due to needing the eosinophils to be at the right level but the diagnosis was determined at about 5 or 6 years old. It was horrible to go so long not understanding why he had so many allergies or why they seemed to change and so on. In his case, he’s essentially allergic to the proteins in a significant amount of foods. We also dealt with constant bronchitis and pneumonia until he finally got on his current treatment about 3 years ago. It was horrible too b/c he would get the same cold as one of us and it’d automatically escalate. He has always had high IGE levels too, which was also crucial for us in getting him diagnosed.
There is just so much and it feels like rambling but it has literally been over 10 years we have dealt with his diagnosis but it is nice to follow and know other journeys too.
Megan Lavin
Welcome. Yes the EOE journey can be such a long and frustrating one. Sending lots of hugs!
Amber
Thank you for some helpful information I didn’t know about. My son is 10 years old and was diagnosed with EOE we are still struggling with the allergy part as well. We think he has had this since her was born. He was put on nutramigen as a baby that help a lot. He would have episodes of swollen lips and hives. As well as vomiting and diraha and severe cramping. We went for years of no one believing us and over looking how severe this was for him. Until we found his Gastro doctor when he was 3 years ago. Even through all his troubles my son still struggles today. I think because he was so much older when we found it out that he’s having a harder time not eating what he shouldn’t. We also have 4 other children and struggle with diet and the cost of his foods he can have. He’s a picky eater at that hard to get to eat fruit and veggies. We still keep pushing for him to try these things but since I have read this I think we need to get back into the allergist to discuss what foods he can have. Thank you for the information . Wish you all well. The saddest part of this all is how people look at my son in school. How bad they treat him when he needs to use the restroom right now or the fact that he’s not happy on some days when he has a flare up etc. it’s constant looks and flares and tolling of eyes when I have to be called to bring in meds or take him home again. Sad to see them I have to be mama bear and be mean and. I have tried to explain what he has for years with teachers principles etc. the school nurse is the nurse for elementary and middle school and I have had it out with her multiple times. Do to her lack of information on his disease it has resorted to her screaming on the top of her lungs to him and looking at him under the door while he’s in the bathroom floor sicker than a dog. Down to them marking him a bad kid. My son also suffers from anxiety disorder which makes things worse. He has been on his meds since he was 7. He does use the budesonide and zertac as well as cyproheptadine as well as a hyoscyamine for cramping. He also has asthma and using inhailers for that too. Nasal sprayer for allergies and constant nasal drip. But I am now going to research an allergist that specializes in EOE thank you again.
Megan Lavin
How sad. I’m so sorry to hear. Sending hugs.
Negar
Dear parents,
Is it possible for a baby to born with EOE?
Recently in 5.5 years old of my son we’ve done andescopy and it showed 5 aesonophils in esophagus in spite of all the diets and pills like Nexium and Telfast and Ranitedin and Zaditen. Does it mean he has EOE?
Does any one know EOE could get away with baby growth?
Your answers to my questions could be a great help to a worried mother. I appreciate you a lot.
Negar
A mother of a son wit great symptoms of allergy that cant sleep too because of reflax.
Kristine
What course of action do you take when an EoE reaction occurs? I’ve been using Benadryl & Pepcid but in extreme cases I go to ER for a Benadryl IV. Has an EpiPen ever helped your son for an EoE episode? I would feel a little more at ease having an EpiPen since my throat closes up & I can’t swallow. However, my allergist said an Epi won’t help. Curious how you handle an EoE attack.
Megan Lavin
Hi Kristine. I can see why that would be confusing for you. As always, taking medications is a medical decision you and your doctor should make. As mentioned in the article, children are less prone to having food stuck, so he’s never experienced that so I’ve never dealt with that first hand. The medications that you mentioned are the ones I’ve heard among other EOE moms as something they do for their kids, but adults symptoms are so different. From the little I understand about an epi pen, I don’t see how that would help food becoming dislodged since epi is adrenaline and helps open the air ways, and as far as I know, it doesn’t dilate the esophagus. I’m sorry, that sounds scary and I hope you can find something that works! If you’re ever scared or in doubt during an episode, the ER is always the place to go. Wishing you safety!
Genevieve
My son was diagnosed with EoE about 2 years ago. He is 8 now. I read your intensely accurate recollection of your sons diagnoses and your family journey. Even though I’m 2 years into his diagnoses I still learned a lot from you! I really did feel so alone and still struggle with that a bit. I’m definitely looking into the APFED conference you spoke about! Thank you, thank you!
Megan Lavin
I’m so glad this was helpful and you could relate. You’re def not alone! 🙂
Harriet Brennan
Thank you for sharing this, this has been so helpful to read. My 20 month old son was just diagnosed with EOE in December and sadly he’s so symptomatic and had become so malnourished we had no choice but to go elemental via feeding tube. We’re awaiting his 2nd scope imminently xx
Megan Lavin
There’s no shame in having to do a feeding tube. I’m so glad you caught it while he was young and wish you the best on the next scope. I’m so glad I could be helpful on your EOE journey.
Madison Haycock
What an informative post. I had no idea this disease existed and I am so impressed with your faith and courage, of you and your whole family. Thank you for sharing!
Megan Lavin
Thanks Madison. It’s my pleasure to share and hope it can help others.
K.C.
My heart goes out to you and to all families that have to endure all the testing and uncertainty. This is a horrible disease, especially in a child. It is good to have family and a community for support.
Megan Lavin
Thanks K.C. Yes, I don’t know what I’d do without the wonderful support we’ve experienced.
Nicole Dawson
My son doesn’t have EOE but after living with life threatening food allergies, going through endless blood work and patch testing, ER visits and using an epi more than 8 times to save him….I feel your pain. You’d provided such great insight and information for anyone with food allergies and I’m sure it will impact many.
Megan Lavin
Eight times Nicole! Holy cow. I’m sorry you’ve had that many scares. I’m sure that was terrifying. It sure takes tough moms to be allergy moms!
Leslie
I can’t even begin to image what you have been through. All of those pin pricks and scopes are hard on both you and your son. Thanks for sharing this.
Megan Lavin
Thanks Leslie. Yes, it was definitely difficult. I’m forever grateful we’re done with the majority of the testing.
Amanda
This was an amazing read. I was unfamiliar with this disease. I’m so glad you were able to get a diagnosis early.
Megan Lavin
Thanks me too. I think the early diagnosis saved us.